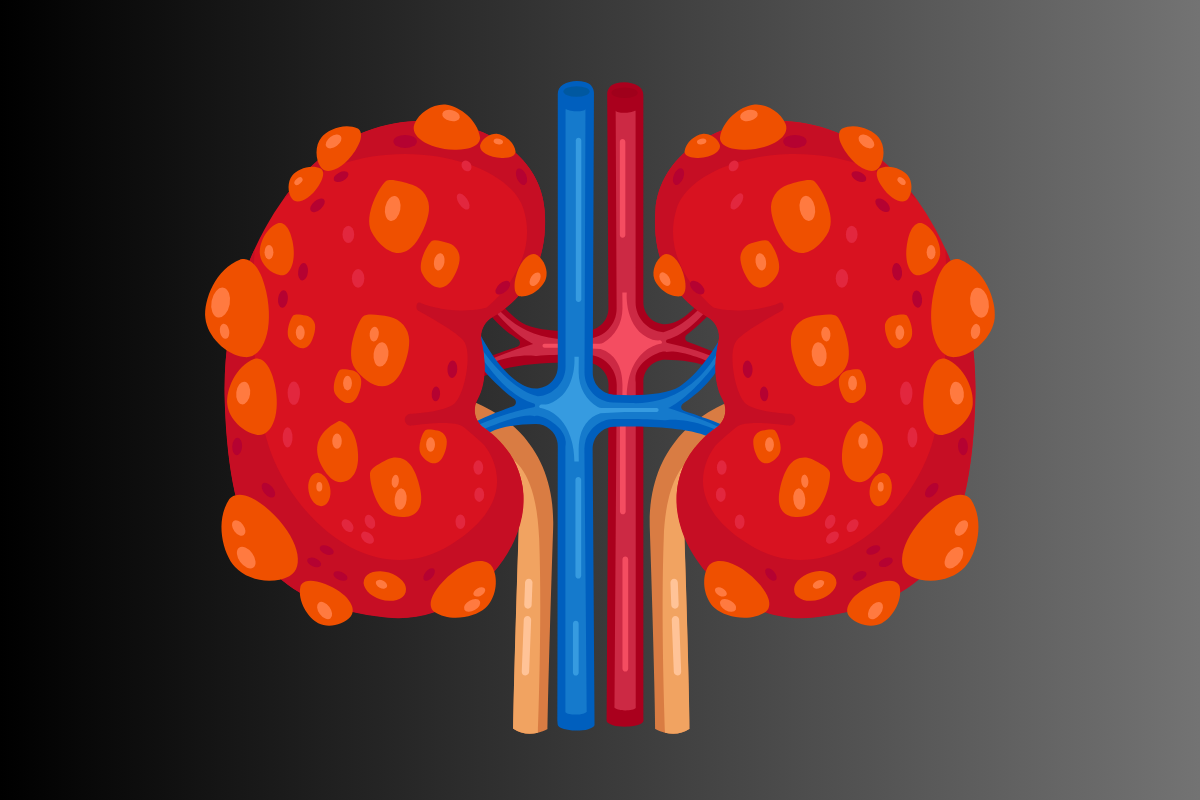
What is Polycystic Kidney Disease (PKD)?
Polycystic Kidney Disease is a genetic condition characterised by multiple fluid-filled cysts in the kidneys which can enlarge and progressively impair kidney function. There are autosomal dominant (ADPKD) and autosomal recessive (ARPKD) forms. Symptoms may be absent early, and appear as cysts grow or kidney function declines.
Common symptoms & signs
- Flank or abdominal pain (dull ache or sharp with cyst complications)
- Blood in urine (hematuria), recurrent urinary tract infections
- Hypertension (high blood pressure)
- Increased abdominal girth, palpable kidney enlargement
- Progressive reduction in urine concentrating ability, and in advanced stages — swelling (edema), fatigue, nausea and reduced appetite
Medical diagnosis & monitoring
Diagnosis is by ultrasound/CT/MRI and family history; kidney function is monitored via serum creatinine, eGFR and urinalysis. Management may include blood pressure control, infection treatment, pain management, cyst interventions and in advanced disease renal replacement (dialysis/transplant). Early medical follow-up and specialist care are essential.
Critical Safety Note
PKD is a potentially serious genetic kidney disease. Ayurvedic therapies below are described as supportive, symptomatic and rehabilitative options that may be considered alongside standard medical care — NOT as replacements for specialist nephrology treatment. Always coordinate with your nephrologist, share labs/imaging, and obtain clearance before starting clinic procedures.
Ayurvedic Perspective & Care Goals
- Ayurvedic view: PKD presentations may be viewed as Vata-Prakopa with Kapha/Ama components causing cyst formation and fluid accumulation; focus is on improving tissue nutrition (Dhatu), reducing Ama (metabolic toxins), supporting renal function (Vrikka/Rakta) and stabilising Vata.
- Practical care goals: Pain relief, reduce infection risk, manage hypertension, support renal tissue nourishment, maintain fluid–electrolyte balance and improve overall quality of life.
- Approach: Individualised combination of internal medicines (liver/kidney-safe herbs), supportive external therapies, lifestyle and diet, with strict medical monitoring.
Clinic Therapies We Use for PKD — with reference images
The therapies listed below are selected for their supportive roles in pain relief, circulation, renal-pelvic comfort, Vata stabilisation and tissue nourishment. Every procedure is individualised and requires medical clearance.
Basti (Medicated Enema) Key
What it is: Therapeutic enemas using medicated oils or decoctions to pacify Vata and nourish pelvic organs.
- Considered central for disorders with Vata imbalance affecting the urinary tract and lower abdomen.
- May help reduce lower-back/flank Vata pain, improve bowel-kidney axis and systemic nourishment.
- Given selectively and only when medically stable; formulations and volumes adjusted for renal safety.
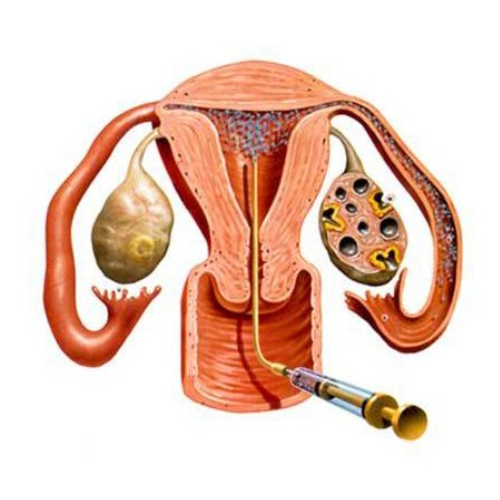
Uttara Basti (Genito-Urinary Instillation) — Selective
What it is: Therapeutic instillation of medicated oil/decoction into the urinary bladder or urethra in specialised settings for local action.
- Used cautiously for selected urinary complaints (recurrent infections, irritative symptoms) after strict assessment.
- Performed only by experienced physicians; contraindicated in acute infection without appropriate medical treatment.
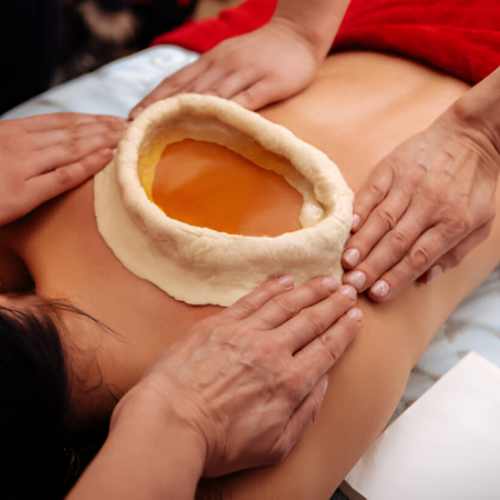
Kati Vasti (Lower Back Oil Retention)
What it is: Warm medicated oil retained over the lower back/lumbar region to relieve pain, stiffness and improve local circulation.
- Often helpful for flank and lower back discomfort associated with enlarged cystic kidneys.
- Reduces muscular tension and supports local tissue nutrition; gentle technique preferred in sensitive patients.
Njavara Kizhi (Nourishing Bolus Therapy)
What it is: Warm boluses of Njavara rice cooked in herb decoction and applied over the body for nourishment and rejuvenation.
- Supports systemic strength, reduces chronic weakness and may improve appetite and tissue repair in recovery phases.
- Used as a rehabilitative measure after acute phases or as part of a long-term restorative plan.
Abhyanga (Warm Oil Massage)
What it is: Gentle full-body herbal oil massage to improve circulation, lymphatic drainage and reduce stress.
- Helps reduce fatigue, improves peripheral circulation and supports detoxification indirectly by improving digestion and sleep.
- Technique and pressure modified for renal patients; frequency individualized.
Kashaya Dhara (Herbal Decoction Pouring)
What it is: Continuous pouring of warm herb decoction over the abdomen or flank to soothe local discomfort.
- Used as a symptomatic measure to ease flank discomfort and improve local circulation with carefully chosen, kidney-safe decoctions.
- Not a substitute for interventions in complicated cysts (infected or bleeding cysts).
Shirodhara (Nervous System & Stress Support)
What it is: Gentle pouring of warm herbal oil on the forehead to calm the nervous system.
- Helpful adjunct for insomnia, anxiety and autonomic imbalance — common in chronic disease contexts like PKD.
- Supports overall well-being and sleep, which are important for chronic disease management.
Herbal Medicines & Nutritional Support (safety first)
Herbal medicines can provide supportive benefits but must be chosen for renal safety and dosed under physician supervision. Some herbs traditionally used to support urinary/renal health are listed below — only after clinician review.
- Gokshura (Tribulus terrestris): Traditionally used for urinary health; dosing must be adjusted in kidney disease and used cautiously.
- Punarnava (Boerhavia diffusa): Diuretic and tissue-supportive in classical texts; use under supervision.
- Varuna (Crataeva nurvala): Traditionally used for urinary tract and bladder support; clinician guidance required.
- Diet: Salt moderation, controlled protein intake as advised by nephrologist, warm easily digestible meals — rice, dal, cooked vegetables, avoid processed foods.
- Avoid: Excessive salt, high-protein fad diets, unnecessary herbal supplements without review, alcohol and nephrotoxic drugs.
- Hydration: Maintain adequate fluid balance per medical guidance (some PKD patients have fluid restrictions in advanced stages).
Any internal herb or supplement must be reviewed for interactions and renal safety (dose adjustment or avoidance may be necessary in reduced kidney function). We always coordinate herb use with the patient's nephrology team and laboratory data.
Sample Clinic Support Plans (examples)
Acute symptom & infection care- Immediate medical evaluation for pain, haematuria or infection
- Treat infections and bleeding under medical guidance; Ayurvedic therapies delayed until stable
- Short supportive Abhyanga (gentle), analgesia coordination with nephrologist
Chronic supportive protocol- Baseline labs & imaging review with nephrology clearance
- Planned series: Basti (selection), Kati Vasti for flank pain, Njavara Kizhi for nourishment
- Adjunct Shirodhara and Kashaya Dhara for symptom relief and stress reduction
Long-term maintenance- Regular monitoring of BP and renal function, diet & lifestyle interventions
- Periodic supportive sessions, individualized herb formulations under supervision
- Coordination for cyst intervention if required (radiologic/surgical) — Ayurveda supports recovery, not surgical decision making
All protocols are tailored. Detoxifying Panchakarma (e.g., strong purgation) is generally not indicated without specialist clearance in PKD; invasive or systemic detox procedures require extra caution in renal disease.
Quick Reference — Therapies & Roles
| Therapy | Primary supportive role | Notes |
|---|
| Basti | Vata pacification, pelvic nourishment | Central supportive therapy; selected use only |
| Uttara Basti | Local genito-urinary support | Very selective; contraindicated in acute infection without medical treatment |
| Kati Vasti | Lower back/flank pain relief | Useful for musculoskeletal support |
| Njavara Kizhi | Rejuvenation, nourishment | Rehabilitative phase use |
| Abhyanga | Circulation, stress reduction | Gentle technique for renal patients |
| Kashaya Dhara | Local soothing & symptomatic relief | Use kidney-safe decoctions only |
| Shirodhara | Stress, sleep & autonomic balance | Adjunctive, improves quality of life |
Need a safe Ayurvedic support plan for PKD?
Book a consultation — we will review your imaging and labs, coordinate with your nephrologist, and design a monitored, stepwise Ayurvedic support plan focused on safety and symptom relief.
Book ConsultationAll procedures are performed by qualified Ayurvedic physicians. Medical clearance (labs, clinician review) is mandatory before interventions.