What is Bladder Control Problem?
Bladder control problems — commonly called urinary incontinence — range from occasional leakage when coughing or sneezing, to a sudden, strong urge to pass urine (urge incontinence) or difficulty fully emptying the bladder. Causes include pelvic floor weakness, nerve dysfunction, chronic infections, prostate issues in men, postnatal pelvic trauma, age-related changes, and Vata imbalance in Ayurvedic terms.
Common types & evaluation
- Stress incontinence: leakage with exertion, cough, sneeze or lifting.
- Urge incontinence: sudden need to urinate with involuntary loss.
- Overflow/retention-related: incomplete emptying causing dribbling.
- Medical evaluation includes urine tests, ultrasound, pelvic exam, uroflowmetry and specialist referral when needed.
Ayurvedic perspective
In Ayurveda, bladder control issues are often considered a manifestation of Apana Vata dysfunction (a Vata subtype governing pelvic organs) with weakness of the pelvic muscle support (Dhatusaithilya) and sometimes Kapha or Pitta factors. Treatment focuses on pacifying Vata, strengthening pelvic tissues, improving local circulation, and restoring neuromuscular control with localized therapies and internal medicines.
Critical Safety Note
If you experience sudden severe urinary retention, blood in urine, fever, painful urination or inability to pass urine, seek immediate medical care. Ayurvedic therapies are supportive and rehabilitative — they should be used after appropriate medical evaluation and in coordination with your physician or urologist.
Ayurvedic Care Pathway (Focused)
- Medical evaluation & coordination: Rule out infection, prostatism, or neurological causes. Urine culture and imaging as needed.
- Pelvic strengthening & local rejuvenation: Therapies to nourish and strengthen pelvic tissues (Uttara Basti, Kati Vasti) and restore Apana Vata.
- Vata-pacifying internal medicines: Herbs and rasayanas that support nerve-muscle function and tissue strength (e.g., Ashwagandha, Bala, Gokshura) — only after clinical assessment.
- Supportive external therapies: Gentle Abhyanga, Udvartana and Njavara Kizhi for systemic nourishment, circulation, and muscle tone.
- Lifestyle & pelvic rehabilitation: Pelvic floor exercises (Kegel), timed voiding, dietary adjustments and weight management.
Therapies We Use for Bladder Control — with reference images
The therapies below are commonly used in clinic protocols for bladder control rehabilitation. Each therapy is individualized; some (like Uttara Basti) require specialized settings and strict indications. Images are provided for clinic reference.
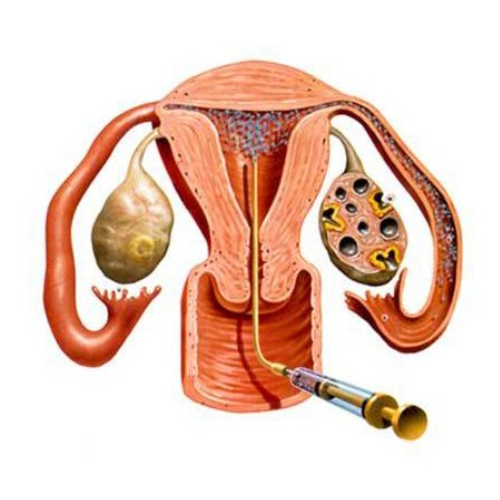
Uttara Basti (Pelvic/Bladder Instillation) Key
What it is: Medicinal oil or decoction administered into the urinary passage under sterile, controlled conditions to nourish and strengthen pelvic tissues.
- Considered a prime localized therapy for pelvic organ weakness, stress incontinence, recurrent urinary complaints and some postnatal cases.
- It helps rebuild mucosal and muscular tone of the lower urinary tract and supports Apana Vata normalization.
- Requires expert administration, sterile technique and urological clearance in many cases.
Basti (Medicated Enema) — Systemic Vata Support
What it is: Medicated oil or decoction administered rectally to pacify Vata and support the gut–pelvic neuroaxis.
- Useful when Apana Vata disturbance is systemic; helps restore coordination of pelvic muscles and nerve reflexes.
- Selected formulations (Anuvasana or Asthapana) are chosen to nourish and tone tissues.
- Given only after assessment — not for acute infection or severe uncontrolled conditions.
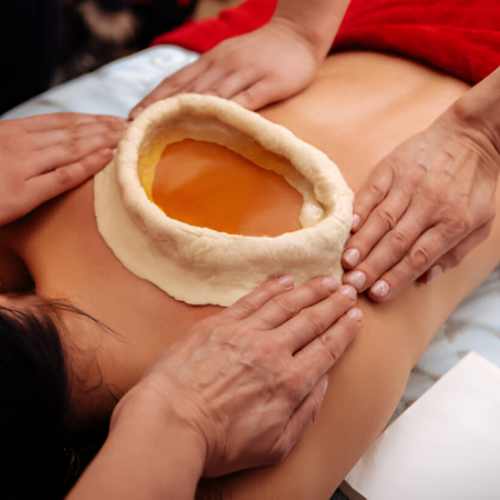
Kati Vasti (Local Oil Retention over Lower Back)
What it is: Warm medicinal oil held over the lower lumbar/pelvic region using a dough ring to improve local circulation and soothe nerves supplying the bladder.
- Targets sacral nerves and pelvic musculature; helps reduce pelvic Vata and improves neuromuscular tone.
- Especially useful for leakage related to pelvic floor weakness or sacral nerve irritability.
Abhyanga (Warm Oil Massage)
What it is: Gentle, rhythmic full-body herbal oil massage to pacify Vata, improve circulation and tone tissues.
- Improves neuromuscular coordination, reduces anxiety and supports systemic strengthening programs.
- Often used before localized therapies to prepare tissues and relax the patient.
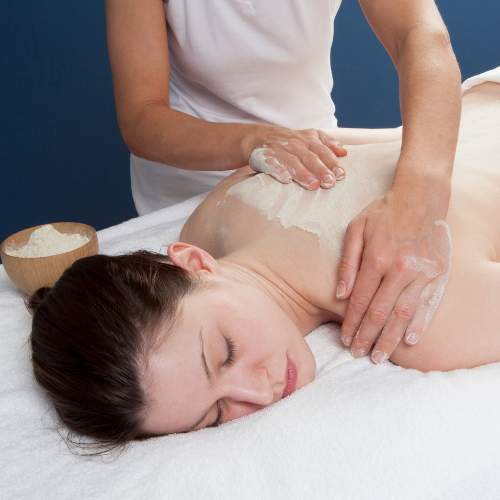
Udvartana (Herbal Powder Massage)
What it is: Vigorous powder massage using specially prepared herbal powders to stimulate local circulation and muscular tone.
- Helps improve pelvic muscle tone and lymphatic drainage when combined with strengthening programs.
- Used carefully in frail or sensitive patients; techniques are adapted per individual tolerance.
Lepam (Herbal Paste Application)
What it is: Application of specific herbal pastes over the lower abdomen or pelvic area to reduce local inflammation and strengthen tissues.
- May be used for soothing local irritation, pelvic congestion and to support tissue repair.
- Formulations are selected to be non-irritant and bladder-safe.
Njavara Kizhi (Rejuvenative Bolus Therapy)
What it is: Warm rice boluses cooked in medicinal decoctions applied to the body to nourish muscles and nerves.
- Useful in rehabilitative phases to rebuild pelvic muscle strength and reduce chronic weakness.
- Often combined with oral rasayanas and pelvic floor exercises for best outcomes.
Herbal Medicines & Nutritional Support
Internal medicines and dietary advice are individualized. Typical supportive options (under physician supervision) include:
- Bala (Sida cordifolia): Strengthening herb used to support muscle and nerve tone.
- Ashwagandha: Nervine tonic and rejuvenator — supports neuromuscular coordination.
- Gokshura (Tribulus terrestris): Traditionally used in urinary and pelvic disorders for tonifying effect.
- Diet: Warm, nourishing, easy-to-digest meals; avoid very cold and excessive diuretics if leakage is present.
- Pelvic rehab: Kegel exercises, timed voiding, bladder training and weight management are essential adjuncts.
- Hydration: Maintain adequate fluids; avoid excess caffeine/alcohol which can worsen urgency.
All herbs and formulations should be prescribed after clinical evaluation, especially when concurrent medical conditions or medications are present.
Sample Clinic Plans (examples)
Initial assessment & stabilization- Medical/urological evaluation to exclude infection or obstruction
- Gentle Abhyanga, pelvic rest guidance & diet modifications
- Start pelvic floor exercise program
Targeted local therapy (after clearance)- Uttara Basti protocol (sterile instillation) when indicated
- Kati Vasti and Lepam for sacral/pelvic support
- Adjunct Njavara Kizhi and selected oral rasayanas to rebuild strength
Maintenance & rehab- Ongoing pelvic physiotherapy, periodic supportive Abhyanga/Udvartana
- Monitoring, lifestyle adjustments and herbal maintenance formulas
Procedures like Uttara Basti require specialist training and are performed only when clinically appropriate and after consent. Coordination with urology/gynecology is recommended when needed.
Quick Reference — Therapies & Roles
| Therapy | Primary role | Notes |
|---|
| Uttara Basti | Local bladder support & mucosal/muscle toning | Specialized, sterile procedure |
| Basti | Correct Apana Vata, neuromuscular coordination | Systemic Vata pacification |
| Kati Vasti | Improve sacral/pelvic circulation & nerve tone | Local oil retention over lower back |
| Abhyanga | General Vata pacification & relaxation | Prepares body for localized therapies |
| Udvartana | Muscle & lymphatic stimulation | Helps pelvic muscle tone |
| Njavara Kizhi | Rejuvenation & strengthening | Used in rehabilitative phase |
Need a safe Ayurvedic plan for bladder recovery?
Book a consultation — we review your investigations, coordinate with your specialist if needed, and design a monitored Ayurvedic program combining local therapies, medicines and pelvic rehabilitation.
Book ConsultationAll procedures are performed by qualified Ayurvedic physicians. Medical/urological clearance may be required before invasive local procedures.