What is Anorexia (Arochaka / Loss of Appetite)?
Anorexia (Ārochaka / loss of appetite) in Ayurveda is commonly due to impaired Agni (digestive fire), Ama (undigested toxins) and dosha imbalance (Vata/Pitta/Kapha patterns). Clinically it shows as reduced desire for food, early satiety, tastelessness, weight loss and weakness. Medical evaluation is important to rule out organic causes (infections, metabolic or psychiatric disorders).
Ayurvedic management emphasizes restoring digestion (Deepana-Pachana), then nourishing (Brimhana/Rasayana) and calming the mind (Satvavajaya). :contentReference[oaicite:4]{index=4}
Red flags — When to seek urgent medical help
- Severe weight loss, fainting, dehydration, syncope, rapid heartbeat, or evidence of an eating disorder (anorexia nervosa) — urgent medical & psychiatric evaluation required.
- Inability to eat for several days, persistent vomiting, or signs of severe malnutrition — seek hospital care.
Ayurveda can be safely integrated as supportive care, but serious medical/psychiatric conditions must be prioritized and managed by appropriate specialists.
Ayurvedic Strategy
- Phase 1 — Deepana & Pachana (ignite digestion & clear Ama): light appetite-stimulating herbs (trikatu, ginger, hing preparations) and digestive routines. :contentReference[oaicite:5]{index=5}
- Phase 2 — Brimhana & Rasayana (nourish & rebuild): therapies and medicines that increase body tissue, weight and strength (e.g., Njavara Kizhi, nourishing medicated ghee formulations, Shatavari/milk preparations).
- Phase 3 — Manasika support: psychological & stress-reducing therapies (Shirodhara, counseling / Satvavajaya) because mental stress often suppresses appetite. :contentReference[oaicite:6]{index=6}
- Gut-brain axis & Vata correction: selected Basti (if Vata predominance or chronic digestive dysregulation) and Nasyam to improve taste/appetite when appropriate.
Clinic Therapies Useful in Anorexia — with reference photos
Only therapies commonly used to improve appetite, nourish tissues and reduce stress are shown below. Each therapy is individualized and performed after assessment.
Deepana & Pachana (Digestive Stimulation)
What it is: Use of appetite stimulants (Deepana) and digestive herbs (Pachana) to rekindle Agni and clear Ama before nourishing therapies.
- Common agents: Trikatu formulations, ginger, hing (asafoetida) and mild carminatives, given in physician-supervised doses. :contentReference[oaicite:7]{index=7}
- Dietary measures: warm, freshly cooked, small frequent meals — spiced gently to support digestion.
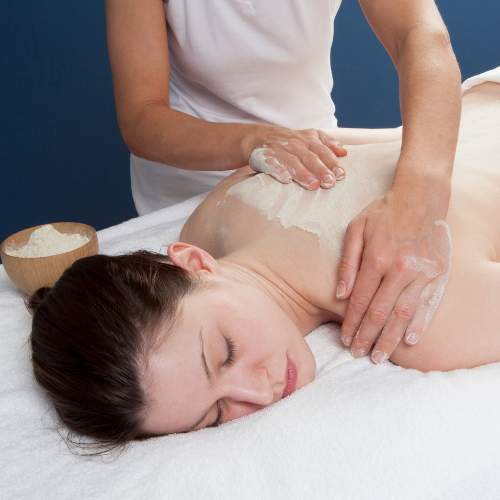
Abhyanga (Warm Oil Massage)
What it is: Gentle full-body massage with nourishing oils (medicated ghee or herbal oils) to reduce Vata, calm the body and improve appetite.
- Prepares the body for deeper nourishing therapies; reduces anxiety and improves sleep which indirectly supports appetite.
Njavara Kizhi (Nourishing Bolus Therapy)
What it is: Warm boluses of Njavara rice cooked in milk/decoction applied to the body to deeply nourish tissues and reverse emaciation.
- Used in the reparative/brimhana phase to rebuild strength, appetite and body tissues after digestion is restored. Evidence and clinical writeups note its anti-emaciation, nourishing effects. :contentReference[oaicite:8]{index=8}
Shirodhara (Stress & Sleep Support)
What it is: Continuous warm oil/medicated liquid flow over the forehead to calm the nervous system.
- Reduces anxiety, improves sleep and lowers physiological stress — useful when lack of appetite is driven by stress or mental factors. Controlled studies report reductions in anxiety markers after Shirodhara. :contentReference[oaicite:9]{index=9}
Nasyam (Nasal Therapy) — Adjunct
What it is: Administration of mild, appetite-friendly oils/powders via the nose to stimulate taste, smell and autonomic balance.
- Can help improve taste and appetite reflexes in select patients; used only after clinical assessment and with liver/gut-safe formulations.
Basti (Medicated Enema) — Selected Use
What it is: Medicated oil or decoction administered rectally to correct chronic Vata, improve gut motility and restore gut-brain balance.
- Selected when Vata predominance or chronic gut dysregulation contributes to appetite loss; always used under physician supervision. Clinical protocols combine Basti with Deepana and Brimhana phases.
Herbs, Dietary & Lifestyle Measures
- Deepana / Pachana herbs: Trikatu (black pepper, long pepper, dry ginger) in physician-supervised doses to kindle Agni and remove Ama. :contentReference[oaicite:10]{index=10}
- Brimhana & Rasayana: Shatavari, Ashwagandha, Vidarikand, medicated ghee (pharmaceutical quality) and milk-based nourishing preparations for rebuilding tissues.
- Formulations: Chyawanprash or physician-formulated rasayanas where appropriate to restore appetite and strength (prescribed case-by-case).
- Diet: Small, warm, freshly cooked, appetizing meals; khichdi, moong dal, light soups, warm milk with nourishing agents; avoid raw, cold or stale foods.
- Routine & environment: Regular meal times, calm eating environment, mindful eating, gentle activity to stimulate appetite (walks, pranayama).
- Psychological support: Satvavajaya (counselling, supportive psychotherapy), family support and when indicated, psychiatric care for eating disorders.
All internal medicines and therapies must be customized by a qualified Ayurvedic physician after a full assessment. For severe or psychiatric anorexia (anorexia nervosa) coordinate with mental health professionals — Ayurveda is supportive but not a substitute for psychiatric care. :contentReference[oaicite:11]{index=11}
Sample Clinic Plans (examples)
Initial (restore digestion)- Medical screening & baseline labs
- Deepana-Pachana herbs, warm small meals, abdominal massage & gentle Abhyanga
- Address dehydration, correct electrolytes if needed
Nourish & rehabilitate- Njavara Kizhi or other brimhana therapies to rebuild tissues
- Medicated ghee preparations, Rasayana, progressive caloric increase
Mental & long-term support- Shirodhara, counseling (Satvavajaya), lifestyle changes and follow-up
- Periodic monitoring and coordination with medical/psychiatric team
Therapies are staged — digestive correction first, then nourishment, then maintenance. In severe cases or where psychiatric diagnosis exists, an integrated approach with conventional medicine is mandatory. :contentReference[oaicite:12]{index=12}
Quick Reference — Therapies & Roles
| Therapy | Primary role | When used / notes |
|---|
| Deepana / Pachana | Restore Agni & clear Ama | First phase — appetite stimulants under supervision. :contentReference[oaicite:13]{index=13} |
| Njavara Kizhi | Rejuvenation & strength | Rehabilitation after digestion is restored. :contentReference[oaicite:14]{index=14} |
| Abhyanga | Reduce Vata, calm body | Supportive and preparatory therapy |
| Shirodhara | Reduce stress / improve sleep | Adjunct when mental factors suppress appetite. :contentReference[oaicite:15]{index=15} |
| Nasyam | Improve taste/appetite reflex | Adjunct in stable patients |
| Basti | Correct chronic Vata, gut-brain axis | Selected use after assessment |
Need a safe Ayurvedic plan to restore appetite?
Book a consultation — we will assess your digestive status, labs (if needed), mental health context, and design a staged Ayurvedic plan focused on safety and nourishment.
Book ConsultationSevere or psychiatric anorexia requires urgent medical & psychiatric evaluation. Ayurveda is supportive and should be integrated with conventional care for serious cases. :contentReference[oaicite:16]{index=16}