What is Liver Cirrhosis?
Liver cirrhosis is a progressive scarring (fibrosis) of the liver resulting from long-term injury (viral hepatitis, alcohol, metabolic liver disease, etc.). It leads to impaired liver function, portal hypertension, ascites, and increased risk of liver failure and complications.
Management focuses on stopping ongoing injury, supporting liver function, managing complications and improving quality of life. Ayurveda offers supportive, hepatoprotective and detoxifying measures that can be coordinated with conventional medical care. :contentReference[oaicite:1]{index=1}
Ayurvedic View & Treatment Goals
Ayurvedic perspective
In classical Ayurveda, chronic liver disease maps to conditions of Yakrit (liver) and Pliha (spleen) dysfunction with involvement of Pitta and Rakta, accumulation of Ama (toxins), and impaired Agni (digestive/metabolic fire). Treatment aims to detoxify, pacify Pitta, purify Rakta, support liver regeneration and strengthen systemic tissues.
Primary clinic goals
- Remove or reduce systemic toxins (Ama) with safe, supervised detox procedures.
- Support hepatocyte health with hepatoprotective herbs and rasayanas.
- Manage complications (ascites, digestion, fatigue) alongside medical specialists.
- Improve nutrition, sleep and overall resilience to slow disease progression.
Evidence & Safety Highlights
Some clinical case series and cohort reports suggest multi-modal Ayurvedic programs (Panchakarma + herbs + diet) can improve symptoms and liver parameters in selected patients with cirrhosis, but evidence is mainly from observational studies and case reports — rigorous randomized trials are limited. Herbal hepatoprotectants (e.g., silymarin/milk thistle) have more clinical trial evidence supporting biochemical improvements in some cirrhosis patients. Always coordinate Ayurveda with hepatology care. :contentReference[oaicite:2]{index=2}
Important safety note: Ayurvedic/herbal products can sometimes cause liver injury or interact with conventional drugs; certain herbs and formulations must be used with caution and medical supervision. Clinical monitoring and lab tests are essential. :contentReference[oaicite:3]{index=3}
How Our Clinic Approaches Cirrhosis (Stepwise)
- Medical assessment & coordination: Baseline labs (LFTs, INR, CBC), imaging and hepatology review. We do not replace indicated medical therapies — we coordinate care.
- Stabilization & diet: Address complications (ascites management, salt restriction) and optimize nutrition before any detox procedure.
- Gentle detox & Panchakarma (selected cases): Mild Virechana or other cleansing methods under strict supervision, only if clinically appropriate.
- Hepatoprotective medicines & rasayanas: Evidence-informed herbs and formulations tailored after clinical review (examples below).
- Supportive therapies: External therapies that improve circulation, reduce congestion and improve patient comfort (listed below with reference photos).
Clinic Therapies Useful in Liver Cirrhosis (with reference photos)
The therapies below are used at our clinic as supportive measures for selected cirrhosis patients (after medical clearance). Each entry includes a therapy photo for quick reference.
Virechana (Therapeutic Purgation)
Use: Carefully selected and mild purgation to eliminate Pitta-related toxins from GI tract and liver regions.
- May be considered in compensated patients after stabilization and preparatory care.
- Helps reduce systemic Pitta/Ama load and improves digestion/metabolism.
- Strict clinical supervision required; contraindicated in decompensated cirrhosis or unstable patients. :contentReference[oaicite:4]{index=4}
Basti (Medicated Enema)
Use: Vata-pacifying and nourishing enemas given in selected protocols to improve systemic balance and gut-liver axis.
- Supports Vata correction and systemic nourishment as part of a wider regimen.
- Only after clinical evaluation; dosing and type of basti customized for liver patients. :contentReference[oaicite:5]{index=5}
Abhyanga (Therapeutic Oil Massage)
Use: Gentle full-body oil massage to improve peripheral circulation, lymphatic flow and patient comfort.
- Helps with malaise, improves sleep and supports gentle detox when used in preparatory/rehabilitation phases.
- Customized oils used based on constitution and liver status.
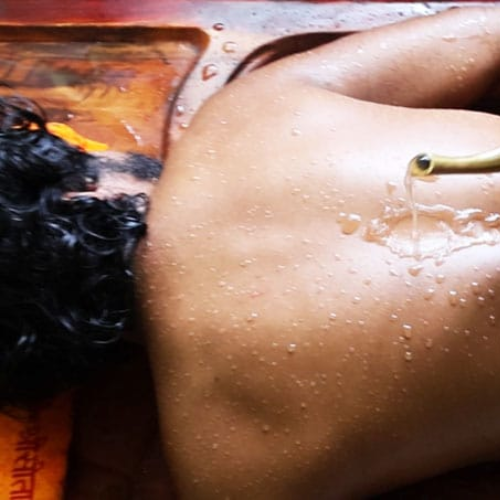
Kashaya Dhara (Herbal Decoction Pouring)
Use: Warm herbal decoctions poured over the abdomen/chest in a controlled manner to soothe tissues and support detox pathways.
- Supportive therapy to relieve congestion and improve local circulation; used with physician oversight.
Oil Bath (Snehana / Rejuvenation)
Use: Full-body oil application or immersion as part of restorative cycles to nourish tissues and improve patient strength.
- Helpful in rehabilitation phases; supports skin, comfort and nutrition absorption.
Shirodhara (Nervous System Support)
Use: Continuous gentle oil pouring over forehead to reduce stress, improve sleep and support neuro-hormonal balance.
- Adjunctive therapy to help restore sleep and resilience — useful for patients with chronic fatigue/insomnia related to liver disease.
Herbal Medicines & Nutritional Support
We select hepatoprotective and rejuvenative herbs/formulations based on clinical assessment. Examples commonly used (individualized dosing & monitoring):
- Kutki (Picrorhiza kurroa): Hepatoprotective, used in detox protocols.
- Punarnava (Boerhavia diffusa): Diuretic/anti-inflammatory helpful for ascites and congestion support.
- Kalmegh (Andrographis paniculata): Bitter, hepatoprotective properties.
- Shilajit / Arogyavardhini (classical formulations): Used in specific rasayana protocols to support recovery.
- Guduchi (Tinospora cordifolia): Traditionally used for liver support — used cautiously and monitored. :contentReference[oaicite:6]{index=6}
- Silymarin / Milk thistle (if used): Evidence from trials shows biochemical benefit in some cirrhosis patients (used as adjunct with medical advice). :contentReference[oaicite:7]{index=7}
- Triphala & digestive tonics: To restore Agni and gentle detoxification.
All herbal medicines are prescribed after lab review. Some Ayurvedic formulations and concentrated herbal extracts have been associated with liver injury in rare cases — careful selection, dose control and monitoring are essential. :contentReference[oaicite:8]{index=8}
Diet, Lifestyle & Medical Monitoring
- Diet: Easily digestible, protein-adequate, low-salt (if ascites), moderate healthy fats (ghee in small amounts if tolerated), no alcohol, avoid raw/ heavy fried foods.
- Fluid & salt management: As per medical advice for ascites/edema.
- Sunlight & activity: Gentle activity as tolerated; maintain muscle mass and mobility with physiotherapy.
- Monitoring: Regular LFTs, coagulation profile (INR), renal function and clinical follow-up while on herbal medicines and procedures.
Sample Clinic Plans (examples)
Stabilize & Support (1–2 weeks)- Medical stabilization, salt/fluid guidance, baseline labs and imaging
- Gentle Abhyanga, nutritional optimization and mild digestive tonics
Detox & Rejuvenation (3–4 weeks — selected cases)- After clearance: preparatory Snehana → mild Virechana (if indicated) → rasayana & hepatoprotective medicines
- Supportive external therapies: Kashaya Dhara, Abhyanga, Shirodhara as tolerated
Maintenance & Monitoring- Monthly supportive therapies, herbal rasayanas, dietary maintenance and regular labs
- Coordinate with hepatology for surveillance (HCC screening, variceal assessment as indicated)
Plans are highly individualized; not every patient is a candidate for Panchakarma/cleansing. All procedures are done only after multidisciplinary review and lab clearance.
Quick Reference — Therapies & Roles
| Therapy | Primary role | Notes |
|---|
| Virechana | Detox Pitta/Ama | Selected cases only; supervised. :contentReference[oaicite:9]{index=9} |
| Basti | Vata pacification & nourishment | Part of internal regeneration protocols. |
| Abhyanga / Oil Bath | Circulation, nourishment | Supportive and preparatory. |
| Kashaya Dhara | Soothing decoction pouring | Adjunctive for tissue comfort. |
| Herbal medicines | Hepatoprotection & rasayana | Silymarin, Kutki, Kalmegh, Punarnava (individualized). :contentReference[oaicite:10]{index=10} |
Selected supporting references & safety notes
Key recent publications and reviews supporting the statements above (representative, not exhaustive):
- Multi-modal Ayurveda management (Panchakarma + medicines) reported to improve clinical profile in cirrhosis case series/cohort reports. :contentReference[oaicite:11]{index=11}
- Silymarin (milk thistle) has randomized trial evidence for biochemical improvements in cirrhosis and is a widely studied hepatoprotectant. :contentReference[oaicite:12]{index=12}
- Systematic reviews of medicinal plants report mixed results; some trials show benefit for liver enzymes but higher-quality evidence is still limited. :contentReference[oaicite:13]{index=13}
- Herbal products can cause liver injury in rare cases; clinical vigilance and lab monitoring are essential. :contentReference[oaicite:14]{index=14}
Want a coordinated Ayurvedic plan for liver support?
Book a consultation — we review tests, coordinate with your hepatologist, and design a safe, individualized program (diet, herbs, and supportive therapies).
Book ConsultationAll therapies are performed by qualified Ayurvedic physicians and are only started after medical clearance and lab monitoring.