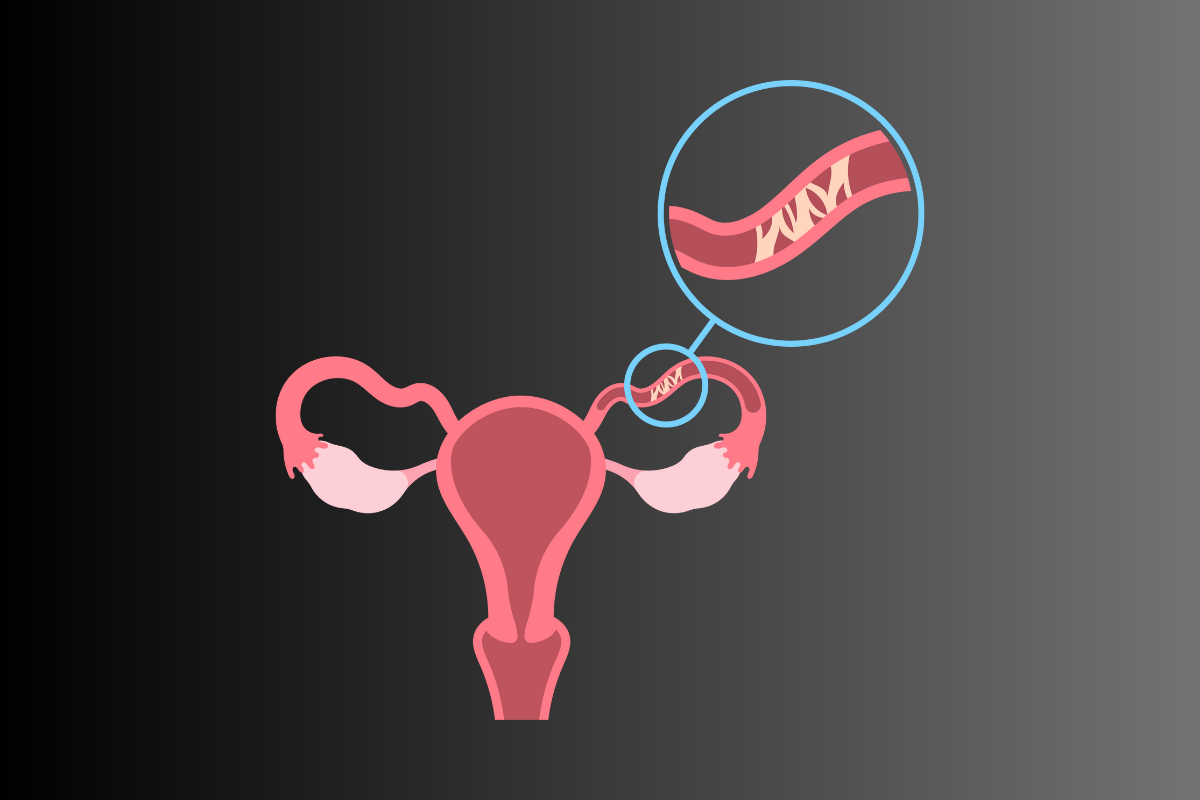
What is Fallopian Tube Blockage?
Fallopian (uterine) tube blockage — partial or complete occlusion of the tubes — prevents egg and sperm meeting and is a major cause of female infertility. Causes include infections (PID), adhesions after surgery, endometriosis, mucus plugs or congenital narrowing. Diagnosis requires imaging (HSG, sonosalpingogram, laparoscopy) and fertility work-up.
Clinical essentials
- Diagnosis: Hysterosalpingography (HSG), sonosalpingography, laparoscopy and fertility testing to confirm tubal patency or obstruction.
- Management: depends on location and cause — some obstructions are amenable to medical/endoscopic/surgical treatment; others may be managed with assisted reproductive technologies (IVF).
Ayurvedic perspective
Classical Ayurvedic texts do not describe 'fallopian tube' as a named structure, but modern Ayurvedic clinicians conceptualize tubal blockage as Sanga/Srotorodha of the Artavavaha/Beejavaha srotas — typically Vata (adhesion/atrophy) with Kapha (obstruction/mucus) involvement. Treatment focuses on clearing Srotorodha (channels), pacifying Doshas, resolving adhesions/mucus, and rejuvenating the reproductive tissues.
Important Safety & Evidence Note
Tubal blockage may require surgical or assisted-reproduction interventions. Ayurveda offers non-surgical, local and systemic therapies (including Uttara Basti, specialized Basti protocols and supportive Panchakarma) that have been reported in case studies and small trials to improve tubal patency and fertility in selected patients. Evidence is mostly from case reports and small clinical studies; results vary and careful coordination with gynecology/infertility specialists is essential before starting therapy. See references for representative studies. :contentReference[oaicite:0]{index=0}
Ayurvedic Care Strategy (overview)
- Medical coordination first: confirm tubal status (HSG / sonosalpingography / laparoscopy) and rule out active infection, ectopic pregnancy risk or urgent surgical indications.
- Acute issues: treat active pelvic infection (with gynecologist) before any intra-uterine procedures; no Uttara Basti during active infection.
- Clear the channels: targeted local therapy — Uttara Basti (intra-uterine/uterine instillation) is the principal local procedure used to cleanse the uterine cavity and assist in removing mucus plugs/intraluminal debris and promote tubal patency in selected cases. :contentReference[oaicite:1]{index=1}
- Systemic detox & channel-clearing: Selected Panchakarma like Virechana and rectal therapies (various Basti protocols — lekhan, anuvasana, niruha) are used to reduce Dosha involvement and promote systemic channel cleansing prior to Uttara Basti in many protocols. :contentReference[oaicite:2]{index=2}
- Rehabilitation: Rejuvenative therapies (e.g., Njavara Kizhi, medicated oils/ghrta internally, Rasayan herbs) to restore endometrial and reproductive tissue health after procedures.
- Monitoring & follow-up: Repeat HSG/sonosalpingogram after therapy cycles to evaluate patency and coordinate with fertility specialists for next steps (timed intercourse, IUI, or IVF if needed).
Therapies Used for Tubal Blockage — with reference images
Listed below are the therapies commonly used in Ayurvedic clinics for selected cases of tubal blockage. All procedures require gynecologic clearance, sterile technique, informed consent and monitoring. Images are provided for reference.
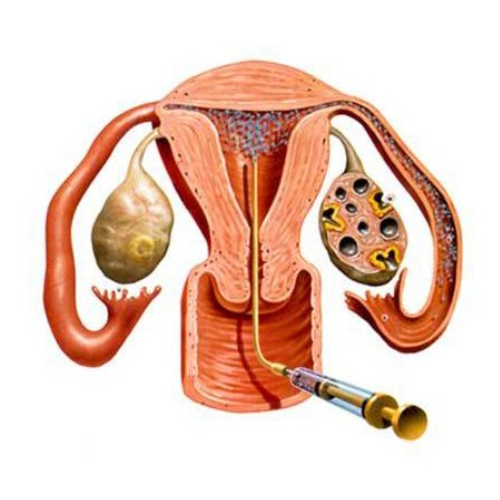
Uttara Basti (Intra-uterine / Intra-vaginal Instillation) Primary
What it is: Sterile intra-uterine or intra-vaginal instillation of medicated oils, ghrita or decoctions (e.g., Kumari Taila, Phala Ghrita, Yavakshara taila) through a controlled uterine route; sometimes called intra-uterine basti.
- Used to cleanse the uterine cavity and reproductive channels, dislodge mucus plugs, reduce adhesions/inflammation, and improve local tissue nourishment.
- Multiple case reports and small clinical studies report improved tubal patency and conception rates after Uttara Basti protocols in selected patients. :contentReference[oaicite:3]{index=3}
- Strict contraindications: active pelvic infection, unassessed pregnancy, heavy bleeding, or compromised uterine anatomy. Must be done under aseptic conditions by experienced practitioners in coordination with a gynecologist.
Basti (Medicated Enema — Lekhana / Anuvasana / Niruha)
What it is: Rectal administration of medicated oils (anuvasana) or decoctions (niruha) designed to pacify Vata, scrape adhesions and clear Srotorodha (channel obstruction).
- Used systemically to reduce Vata-related adhesions and promote gut–reproductive tract axis health; often part of a multi-step protocol (preparatory snehapana → svedana → basti → uttara basti). :contentReference[oaicite:4]{index=4}
- Choice of basti (lekhan, anuvasana, etc.) is tailored to the patient’s dosha, strength and pathology.
Virechana (Therapeutic Purgation)
What it is: Controlled herbal purgation to eliminate aggravated Pitta and systemic toxins, often used as preparatory Shodhana before local procedures.
- Used in Pitta-dominant or mixed patterns where systemic detox is necessary prior to Uttara Basti and basti protocols. It may help reduce inflammatory components contributing to tubal pathology. :contentReference[oaicite:5]{index=5}
- Requires careful patient selection, hydration and lab monitoring.
Abhyanga (Warm Oil Massage) — Supportive
What it is: Gentle, nourishing full-body massage with selected medicated oils to improve circulation, reduce stress and prepare the body for detox procedures.
- Supports systemic nourishment, reduces Vata imbalance and prepares tissues for deeper therapies.
Njavara Kizhi (Rejuvenative Bolus Therapy)
What it is: Warm njavara rice boluses cooked in herbal decoctions applied to the body to rebuild tissues and strength after invasive procedures.
- Used in the recovery/rasayana phase to support endometrial & reproductive tissue health after clearing procedures.
Shirodhara — Supportive (Sleep & Stress)
What it is: Warm oil or decoction poured continuously on the forehead to calm the nervous system, reduce stress and improve sleep, which supports fertility outcomes.
Herbal Medicines & Supportive Measures
Oral medicines and local formulations are selected by the treating Ayurvedic physician. Below are commonly used measures reported in clinical practice and case studies — each must be prescribed with care and gynecologic coordination.
- Local oils/ghritas for Uttara Basti: Kumari Taila, Phala Ghrita, Yavakshara Taila, Apamarga Kshara Taila (selected per protocol in studies). :contentReference[oaicite:6]{index=6}
- Systemic herbs: Rasayan (rejuvenative) formulas and hepatoprotective & nutritive herbs as needed (to support systemic health and reproductive tissue regeneration).
- Anti-adhesive & scraping preparations: Lekhana (scraping) formulations used in basti protocols to address adhesions as per clinical tradition and case protocols. :contentReference[oaicite:7]{index=7}
- Diet & lifestyle: Warm, easily digestible, nutrient-dense foods; avoid cold/raw heavy meals, excessive stimulants and alcohol. Promote restful sleep and stress reduction.
- Infection control: Ensure infections (e.g., PID) are fully treated with conventional care before local uterine instillation or invasive procedures.
Clinical evidence is largely case-based and from small clinical series; outcomes vary by cause, site of blockage (proximal vs distal), extent of adhesions and individual patient factors. Shared decision-making with fertility specialists is essential. :contentReference[oaicite:8]{index=8}
Sample Clinic Plans (examples)
Assessment & Stabilization- Full fertility work-up (HSG/sonosalpingogram), infection screening
- Treat active infections with gynecologic team before any local procedures
- Baseline counseling and informed consent
Shodhana & Channel Preparation- Gentle systemic preparatory measures (Snehapana, Svedana as needed)
- Virechana and tailored Basti protocol (lekhana/anuvasana/niruha) to reduce dosha imbalance and Srotorodha
- Monitor labs and patient strength
Local Therapy & Rehabilitation- Uttara Basti cycles (sterile technique) using appropriate medicated oils/ghrita
- Post-procedure rejuvenation (Njavara Kizhi, rasayana), repeat HSG after treatment cycle to assess patency
- If patency improves — plan fertility management (timed intercourse / IUI); if not, discuss IVF/surgical options
All plans individualized — document informed consent, sterile technique, and cross-specialty communication for best outcomes.
Quick Reference — Therapies & Roles
| Therapy | Primary role | Notes |
|---|
| Uttara Basti | Local cleansing of uterine/tubal channels; dislodge plugs and reduce adhesions | Primary local procedure; multiple case reports show improved patency in selected patients. :contentReference[oaicite:9]{index=9} |
| Basti (Lekhana / Anuvasana / Niruha) | Systemic channel clearing, anti-adhesive effects | Used in preparatory protocols to reduce Vata/Kapha obstruction. :contentReference[oaicite:10]{index=10} |
| Virechana | Systemic detox for Pitta component | Supportive preparatory Shodhana in selected patterns. :contentReference[oaicite:11]{index=11} |
| Njavara Kizhi | Rejuvenation & tissue nourishment | Used in rehabilitation to improve strength and endometrial health. |
| Abhyanga / Shirodhara | Supportive nourishment, stress & sleep | Adjuncts to aid overall recovery and fertility readiness. |
Considering Ayurvedic care for tubal blockage?
Book a multidisciplinary consult — we’ll review your fertility reports, coordinate with your gynecologist, and design a monitored, evidence-aware Ayurvedic plan. Treatment decisions are individualized and safety-first.
Book ConsultationUttara Basti and localized uterine procedures must be done sterilely by qualified clinicians and are contraindicated during active pelvic infection or pregnancy.