Lepam (Medicated Pastes)
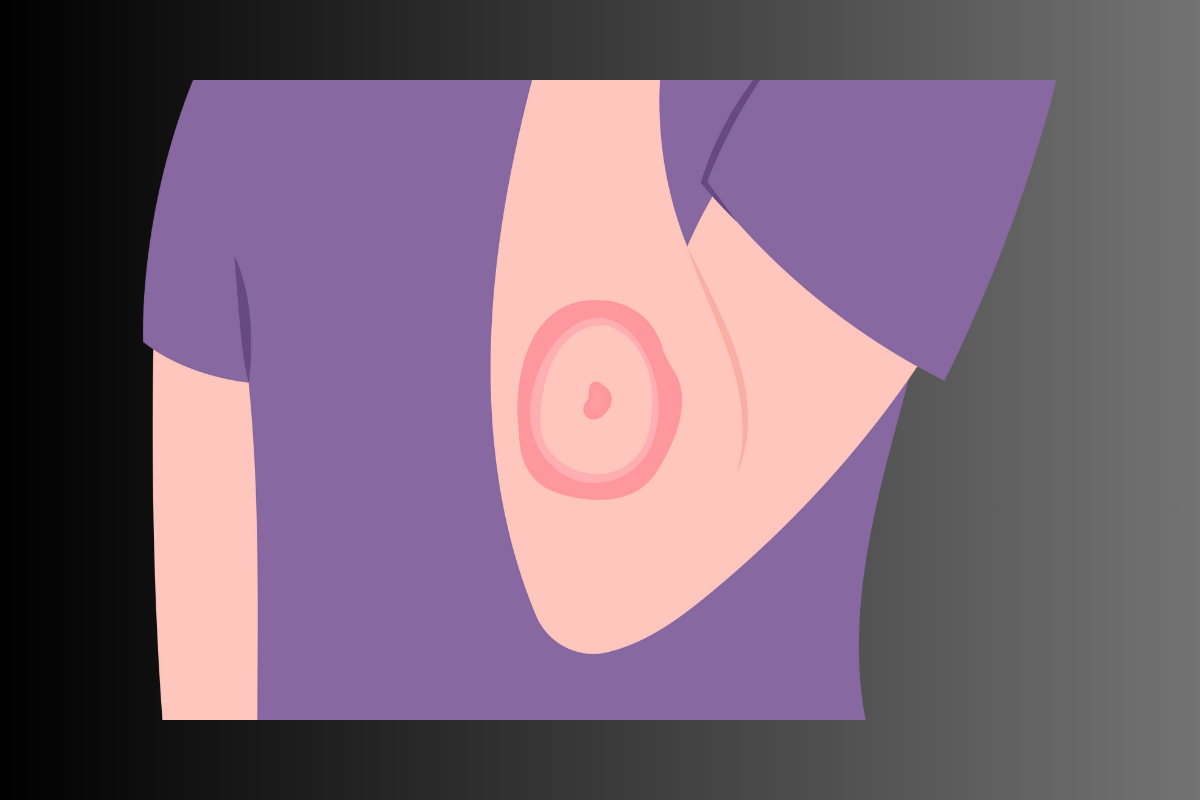
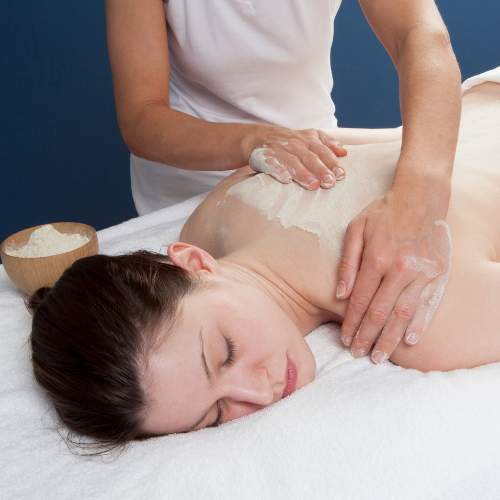
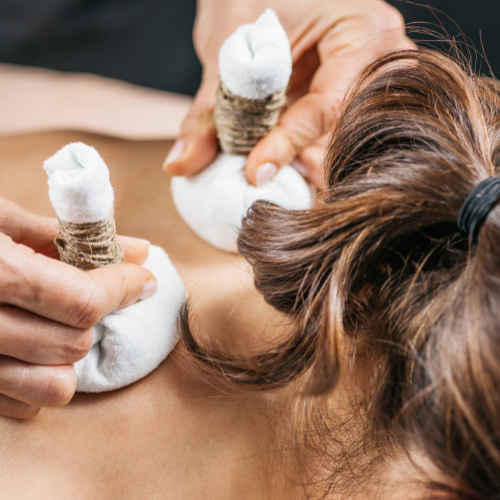
What it is: Topical application of herbal pastes (e.g., neem, turmeric, manjistha, neem+turmeric in a suitable base) directly onto lesions.
- Antifungal, antiseptic and soothing — reduces scaling, itching and local inflammation.
- Applied for a defined time, then gently washed off; repeated daily or as prescribed.
- Formulations chosen to avoid photosensitising or irritant herbs on sensitive skin.