What is Urinary Incontinence?
Urinary incontinence is involuntary leakage of urine. It ranges from occasional small leaks to complete loss of bladder control. Common types include stress incontinence (leak with cough/sneeze/exertion), urge incontinence (sudden need to pass urine), mixed, and overflow incontinence. Causes include pelvic floor weakness, nerve injury, urinary tract conditions, obesity, chronic cough, childbirth, aging and some medications.
Common symptoms & evaluation
- Symptoms: leakage with effort, urgency with little warning, frequent urination, nocturia (nighttime urination).
- Important evaluation: medical history, physical & pelvic exam, urine tests, post-void residual measurement, and urology referral where needed.
- Rule out infections, uncontrolled diabetes, neurological disease or structural problems before starting focused therapies.
Ayurvedic perspective
In Ayurveda urinary incontinence is commonly associated with Mutraghata and Vata imbalance (particularly Apana Vata) causing loss of normal force of retention. Treatment targets pacifying Vata, strengthening pelvic tissues and restoring proper Apana function via local therapies, internal medicines and lifestyle/dietary measures.
Critical Safety Note
Always obtain medical assessment to exclude infections, stones, neurological causes or serious urological conditions before starting Ayurvedic therapies. We work with medical teams for diagnosis and monitoring. Some procedures (like Uttara Basti) require experienced clinicians and sterile technique.
Ayurvedic Care Pathway (Focused)
- Medical screening & coordination: Urine analysis, ultrasound or specialist referral when indicated.
- Vata pacification & tissue strengthening: Therapies aimed at restoring Apana Vata and toning pelvic tissues.
- Local treatments: Uttara Basti and Kati/Prishtha Vasti to directly support pelvic/low-back regions and bladder function.
- Systemic rejuvenation: Njavara Kizhi, Basti (selective) and nourishing oils/medicines to improve muscle tone and neuromuscular control.
- Rehab & lifestyle: Pelvic floor exercises, weight optimization, bladder training, dietary modifications and herbs to support tissue repair.
Therapies We Use for Urinary Incontinence — with reference images
Below are the clinic therapies most useful for urinary incontinence. Each entry includes a reference photo. Therapies are individualized and require clinician assessment and, where needed, sterile procedure settings (e.g., Uttara Basti).
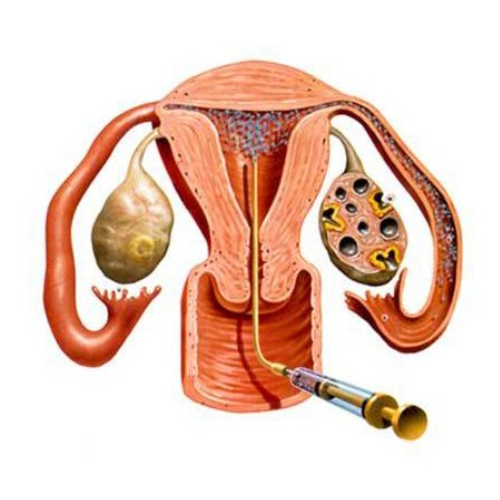
Uttara Basti (Therapeutic Instillation) Primary
What it is: Medicinal oil or decoction instilled into the urinary tract (vaginal/urethral) or bladder region under professional supervision to strengthen pelvic tissues and restore continence mechanisms.
- Directly addresses Apana Vata and local tissue weakness—used for persistent stress/urge incontinence patterns after evaluation.
- Requires sterile technique, experienced practitioner and prior preparation (outer oleation/steam when indicated).
- Given as a course of sessions with monitoring of symptoms and urinary health.
Basti (Medicated Enema) — Selected Use
What it is: Rectal administration of medicated oils or decoctions to pacify Vata (especially Apana) and restore gut-pelvic neuromuscular tone.
- Considered a cornerstone for Vata-related pelvic dysfunction—improves neuromuscular coordination and pelvic support.
- Prescribed based on patient stability and performed under clinician supervision as part of a sequence (including preparatory measures).
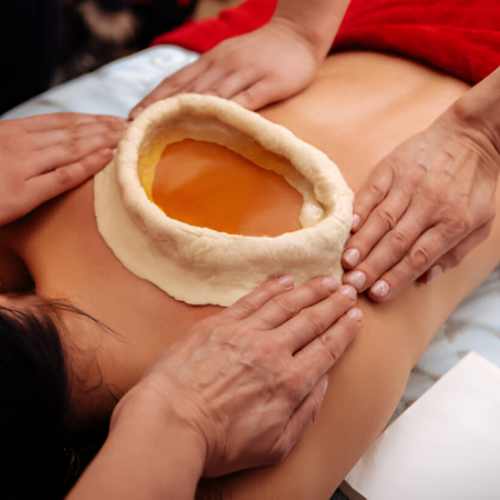
Kati Vasti (Localized Lower Back Oil Retention)
What it is: Warm medicated oil retained over the lower back/pelvic area in a dough-wall reservoir to nourish local tissues and relieve nerve/low-back contributions to incontinence.
- Supports sacral nerve function, reduces local Vata imbalance and eases low-back discomfort that often coexists with pelvic floor weakness.
- Given as a series to strengthen the pelvic-lumbar region.
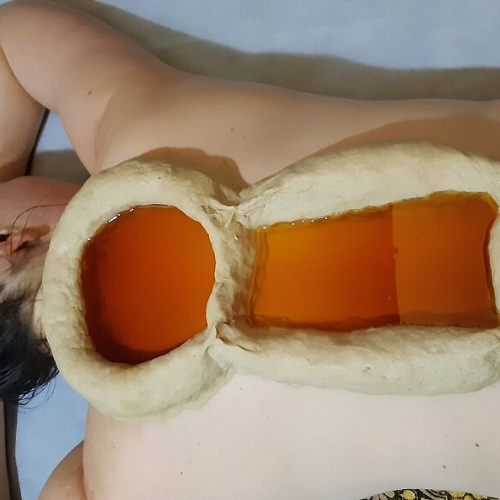
Prishtha Vasti (Back Region Oil Retention)
What it is: Similar to Kati Vasti but applied to the sacral/upper gluteal area to target nerves and muscles involved in bladder control.
- Useful when sacral nerve irritation or lower back Vata contributes to poor bladder control.
- Often combined with strengthening and internal medicines for better outcomes.
Njavara Kizhi (Nourishing Bolus Therapy)
What it is: Warm boluses of Njavara rice cooked in medicated decoctions applied to the body to provide systemic nourishment and strengthen musculature.
- Helps rebuild pelvic muscular tone and general vitality—particularly useful in post-partum or weakness-related incontinence.
- Given during the rehabilitative phase alongside pelvic exercises and tonic herbs.
Abhyanga (Warm Oil Massage)
What it is: Gentle full-body herbal oil massage to pacify Vata, improve circulation and prepare the body for local therapies.
- Supports relaxation, reduces nervous excitability and improves muscular responsiveness when combined with targeted therapies.
- Used as preparatory care ahead of Basti/Uttara Basti or as supportive maintenance.
Lepam (Medicated Paste Application)
What it is: Topical application of medicated pastes over the lower abdomen or perineal region to provide local strengthening and reduce irritation.
- Can be used to locally nourish and tonify tissues when chosen formulations are safe and non-irritating.
- Often part of combined local therapy sessions.
Shirodhara (Nervous System Support)
What it is: Continuous pouring of warm herbal oil on the forehead to calm the nervous system and reduce stress-related urinary urgency.
- Helpful when urge incontinence has a strong nervous/psychogenic component or when stress worsens leakage.
- Used as adjunctive therapy to improve sleep and autonomic balance.
Herbal Medicines & Supportive Measures
Internal medicines and nutritional advice are chosen to safely support strengthening and Vata pacification. All internal prescriptions are personalized and coordinated with the patient's medical status.
- Herbs commonly used (selected & monitored):
- Yashtimadhu (Licorice) — trophorestorative in appropriate doses and formulations.
- Kapikacchu (Mucuna) & strengthening rasayanas — used selectively under supervision.
- Ashwagandha — neuro-muscular support and rejuvenation in rehabilitative phase.
- Diet & lifestyle: Warm, nourishing foods; avoid excessive diuretics (coffee, alcohol). Include protein (lentils, dairy if tolerated), warm soups and stewed vegetables to rebuild tissue.
- Exercises: Pelvic floor (Kegel) exercises, guided physiotherapy, bladder training and weight management are integral to outcomes.
- Behavioral: Timed voiding, avoiding bladder irritants (citrus, caffeine), and smoking cessation if relevant.
If infection, significant post-void residual or neurological disease is present, medical/urological management is prioritized. Ayurveda is complementary and rehabilitative.
Sample Clinic Plans (examples)
Acute assessment & stabilization- Medical screening: urine culture, ultrasound, post-void residual.
- Treat infections or reversible causes first.
- Begin gentle Abhyanga, diet modification & pelvic floor advice.
Rehabilitation & targeted therapy- Course of Uttara Basti (where indicated) + supportive Basti if Vata-dominant.
- Kati/Prishtha Vasti and Njavara Kizhi for sacral support and strengthening.
- Pelvic physiotherapy & bladder training alongside internal tonics.
Maintenance & follow-up- Periodic supportive sessions (Abhyanga, Lepam) and exercise reinforcement.
- Long-term lifestyle & dietary guidance to prevent recurrence.
- Coordinate with urogynecology/urology for mixed or refractory cases.
All invasive procedures (Uttara Basti, certain Basti protocols) are only performed by experienced clinicians with appropriate informed consent and sterile procedure rooms.
Quick Reference — Therapies & Roles
| Therapy | Primary role | Notes |
|---|
| Uttara Basti | Direct pelvic instillation — restore continence mechanisms | Primary therapy for pelvic weakness (sterile, skilled). |
| Basti | Pacify Apana Vata, improve neuromuscular tone | Systemic Vata correction; selected use. |
| Kati / Prishtha Vasti | Local sacral/lumbar support, nerve conditioning | Targets sacral nerves and muscles. |
| Njavara Kizhi | Rejuvenation & tissue strengthening | Good for post-partum weakness and rebuilding tone. |
| Abhyanga & Lepam | Preparation, nourishment, local toning | Supportive and preparatory therapies. |
| Shirodhara | Autonomic & stress regulation | Adjunct where urgency has strong stress component. |
Need a stepwise Ayurvedic plan for urinary incontinence?
Book a consultation — we'll review your medical tests, coordinate with specialists if needed, and design a monitored, stepwise Ayurvedic rehabilitation plan tailored to your type of incontinence.
Book ConsultationAll procedures are performed by qualified Ayurvedic physicians. Medical clearance and appropriate tests are mandatory before invasive therapies.